Health
NACA Issues Warning: New HIV Injection Lenacapavir Unsafe for Pregnant Women
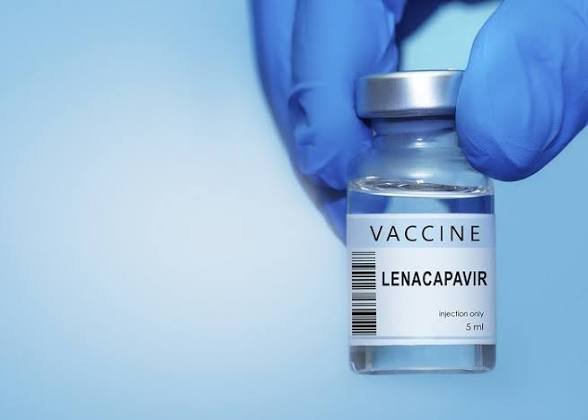
The National Agency for the Control of AIDS (NACA) has cautioned that the newly introduced twice-yearly HIV prevention injection, Lenacapavir, is not recommended for pregnant women due to insufficient safety data.
Director-General of NACA, Temitope Ilori, gave the advisory on Monday during a media briefing in Abuja, organised by the National HIV, Viral Hepatitis and Sexually Transmitted Infections Control Programme under the Federal Ministry of Health and Social Welfare.
“Even though LenPrEP is considered very safe based on global studies, it is not recommended for pregnant women,” Ilori said, stressing that the drug is strictly for prevention known as pre-exposure prophylaxis (PrEP) and not for treating existing HIV infections.
The drug, Lenacapavir, developed by Gilead Sciences, is administered via injection twice a year and is seen as a major breakthrough in HIV prevention, especially for individuals who struggle with daily oral PrEP adherence. Clinical trials have shown near-total protection against HIV among high-risk groups.
Nigeria recently received 11,520 doses through support from the Global Fund, marking the beginning of a phased nationwide rollout. Preparations, including regulatory clearance by National Agency for Food and Drug Administration and Control (NAFDAC), healthcare worker training, and community sensitisation, are already underway.
National Coordinator of the programme, Adebobola Bashorun, said efforts are ongoing to expand access, particularly among vulnerable populations.
“As we scale up, we are exploring catalytic funding to increase doses and reach those most at risk,” he said, adding that Lenacapavir will complement existing prevention tools rather than replace them.
Bashorun noted that reported side effects have been mild, mainly injection-site reactions such as pain or swelling, while authorities continue close monitoring for any adverse outcomes.
Minister of State for Health, Iziaq Salako, attributed the availability of the drug to partnerships with global donors and expressed optimism about future local production through technology transfer.
Despite its promise, officials warned that Lenacapavir does not protect against other sexually transmitted infections, including hepatitis, syphilis, or gonorrhoea. Users are therefore advised to maintain safer-sex practices, including condom use.
Nigeria continues to bear a significant HIV burden, with about 1.9 million people living with the virus and an adult prevalence rate of roughly 1.3%. While treatment coverage has improved, prevention gaps remain, particularly among young people and key populations.
Health authorities describe Lenacapavir as a potential “game-changer” in reducing new infections but stress that its success will depend on equitable access, sustained funding, and effective integration into the country’s broader HIV response strategy.
Health
Nigerian Dietitian Dismissed in UK Over False Qualifications, Competency Concerns

A Nigerian-born senior dietitian, Ifeyinwa Chizube Ndulue-Nonso, has been dismissed from her role in the United Kingdom after a tribunal found she misrepresented her qualifications and demonstrated serious gaps in basic medical knowledge.
Ndulue-Nonso was employed by Manchester University NHS Foundation Trust in February 2024 after scoring 62 percent during her interview. However, concerns about her competence reportedly surfaced within days of resuming duty.
According to tribunal findings, she admitted to exaggerating her experience during the hiring process, stating she had “lied over her qualifications a bit,” which she attributed to cultural differences.
Her supervisor, Lorna Haywood, raised alarm over what she described as “extremely concerning” knowledge gaps, noting that the issues involved fundamental aspects of human anatomy and clinical practice.
Among the reported errors, Ndulue-Nonso allegedly stated that urine is stored in the gallbladder and that radiotherapy is used to treat heart failure. She was also said to have struggled with calculating body mass index (BMI) and incorrectly identified parts of the digestive system.
Further concerns emerged when she reportedly admitted to lacking practical experience in key procedures she had claimed familiarity with, including intravenous feeding and the use of nutritional supplements. She was also said to have failed to recognise a feeding tube in a patient and was observed searching online for basic medical terms during work hours.
She was suspended in March 2024 pending an investigation into her credentials. Disciplinary proceedings later found that 20 out of the 28 areas of expertise she claimed were not supported by her actual knowledge or experience.
Following the outcome, she has been barred from practising as a registered dietitian in the UK.
The case has raised broader concerns about recruitment processes and verification of professional qualifications in the healthcare sector.
General News
Jehovah’s Witnesses Ease Rules On Blood Transfusions Allow Use Of Own Blood
Jehovah’s Witnesses has updated its long standing policy on blood transfusions, now allowing members to have their own blood removed, stored, and later returned during medical procedures.
The adjustment means adherents can undergo planned surgeries involving the use of their own blood, but the group still prohibits receiving blood donated by others.
Gerrit Losch, a member of the movement’s leadership, announced the change, stating that each individual Christian must decide how their blood is used in medical and surgical care.
Despite the revision, the organisation emphasized that its core belief on the sanctity of blood remains unchanged. The doctrine is rooted in interpretations of biblical teachings, which followers say instruct believers to abstain from blood.
The development has drawn mixed reactions. Some former members argue the update does not go far enough, particularly in emergency situations where donated blood may be required to save lives.
In a recent legal case in Edinburgh, a court ruled that doctors could administer a blood transfusion to a 14 year old Jehovah’s Witness if necessary to preserve her life, despite her refusal on religious grounds. The judge held that such intervention would be in the child’s best interest.
Jehovah’s Witnesses, known globally for their door to door evangelism, number about nine million members worldwide, including roughly 144,000 in the United Kingdom.
Health
Alberta Moves to Restrict Medically Assisted Dying to End-of-Life Cases
Alberta has proposed new legislation to limit the use of medically assisted dying (MAID) strictly to patients at the end of life, marking the first time a Canadian province has independently sought to impose such restrictions.
Currently, Canada allows medically assisted dying for individuals with serious, incurable illnesses or disabilities, even if their death is not reasonably foreseeable. Federal law is also set to expand MAID eligibility next year to include those whose sole medical condition is mental illness, though implementation has already been delayed twice.
Speaking at a news conference on Wednesday, Alberta Premier Danielle Smith emphasized that assisted dying should be reserved for those with no hope of recovery. “This legislation strengthens safeguards and restores clear limits on eligibility to protect vulnerable Albertans facing mental illness or living with disabilities,” she said. “Those struggling with severe mental health challenges need treatment, compassion and support, not a path to end their life at what may be their lowest moment.”
The proposed bill would prohibit doctors from initiating MAID discussions with patients and ban public advertising of the service in healthcare facilities. It would also formalize conscience protections for healthcare professionals and institutions.
Supporters of the legislation include Moira Wilson, president of Inclusion Canada, who said it “demonstrates that governments can strengthen laws and better protect people whose lives are not nearing an end,” and Mara Grunau, CEO of the Canadian Mental Health Association’s Alberta division, who highlighted the importance of recovery from mental illness.
However, opponents, including Helen Long, CEO of Dying with Dignity Canada, argue the proposal undermines patient autonomy. Long described the legislation as “a direct attempt to circumvent the constitutional criminal law authority” and warned it could create additional barriers for suffering individuals wishing to exercise choice.
Medically assisted deaths currently account for roughly 5% of deaths in Canada, with the majority involving patients whose death was reasonably foreseeable. Alberta’s proposed law aims to ensure that vulnerable groups, particularly those with mental illnesses or disabilities, are offered support and care rather than premature death.
Canada is among a handful of countries that have introduced assisted dying laws in the past decade, including Australia, New Zealand, Spain, and Austria.
